Click here to read the Marathi article: एपिलेप्सी (अपस्मार)
The brain is made up of billions of nerve cells called neurons that create electrical signals to communicate with one another. A seizure occurs when there is abnormal and overactive electrical activity of brain cells. The seizure may include brief stares and muscle spasms (shaking, lip smacking). Some people have strange or odd sensations (bad smells, unusual or bad tastes, and changes in vision) right before they have a seizure. This “warning” sign of a seizure is called an aura.
Not all body shaking is caused by seizures and not all seizures are body shaking!
Causes of seizures: A seizure can be a symptom of another health problem, such as:
- A rapidly increasing fever (fever seizure or febrile seizure).
- An extremely low blood sugar level.
- Brain surgery or a head injury.
- Withdrawal from alcohol, prescription medicine, or illegal drugs.
- An infection, such as meningitis or encephalitis.
- Parasitic infections, such as tapeworm or toxoplasmosis.
- Electrolytes like low sodium or low calcium level in blood.
Unprovoked seizure– a seizure that occurs in the absence of above-mentioned conditions.
At least two unprovoked seizures occurring more than 24 hours apart is known as epilepsy. Epilepsy is a brain disorder that causes seizures. It is also called a seizure disorder. The cause of epilepsy may not be known. If the seizures are not controlled, epilepsy may become life-threatening. A seizure may last a few seconds or longer than 5 minutes. The risk of epilepsy is higher with a family history of epilepsy.
- Number of people around the world who have epilepsy: 65 million
- Number of people in the United States who have epilepsy: 3.4 million
- Number of new cases of epilepsy in the United States each year: 150,000
There are three phases to a seizure. They are:
- Pre-Ictal: the time period before a seizure. The person may feel or behave differently from normal.
- Ictal: the time during the seizure, when seizure activity is actually happening.
- Post-Ictal: the time period after a seizure. The person may be confused, not know their name or where they are, and may need time to rest and often sleep.
Types of seizures:
Partial or focal seizures: affects only one area or one side of the brain. They can be
- Simple partial seizures– These seizures can cause twitching or a change in sensation, such as a strange taste or smell.
- Complex partial seizures– can make a person confused or dazed. The person will be unable to respond to questions or direction for up to a few minutes.
- Secondary generalized seizures– begin in one part of the brain, but then spread to both sides of the brain.
Generalized seizures: affect both sides of brain. There are several types of generalized seizures.
- Generalized tonic clonic seizures (GTC)- also called grand mal seizures, can make a person cry out, lose consciousness, fall to the ground and have muscle jerks or spasms.
- Myoclonic seizures-sudden and brief muscle jerks
- Atonic seizures or drop seizures- child loses muscle tone and falls
- Absence seizures or petit mal seizures- rapid blinking or a few seconds of staring into space without being aware of his/her surroundings.
- Tonic seizures– stiffening of hands and legs
Causes of epilepsy1:
Epilepsy has no identifiable cause in about half the people with the condition. In the other half, the condition may be traced to various factors, including:
- Genetic influence. Some types of epilepsy run in families. It is likely to be genetic in nature. Researchers have linked some types of epilepsy to specific genes, but for most people, genes are only part of the cause of epilepsy. Certain genes may make a person more sensitive to environmental conditions that trigger seizures.
- Head trauma. Head trauma as a result of a car accident or other traumatic injury can cause epilepsy.
- Brain conditions. Brain conditions that cause damage to the brain, such as brain tumors or strokes, can cause epilepsy. Stroke is a leading cause of epilepsy in adults older than age 35.
- Infectious diseases. Infectious diseases, such as meningitis, AIDS and viral encephalitis, can cause epilepsy.
- Prenatal injury. Before birth, babies are sensitive to brain damage that could be caused by several factors, such as an infection in the mother, poor nutrition or oxygen deficiencies. This brain damage can result in epilepsy or cerebral palsy.
- Developmental disorders. Epilepsy can sometimes be associated with developmental disorders, such as autism spectrum disorder and neurofibromatosis.
How is epilepsy diagnosed?
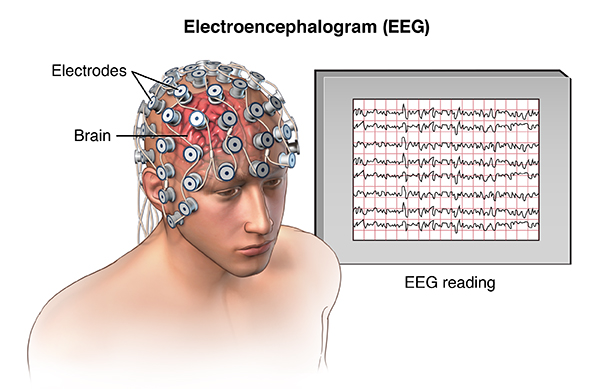
- An electroencephalogram (EEG) records the electrical activity of the brain. It is used to find changes in the normal patterns of brain activity.

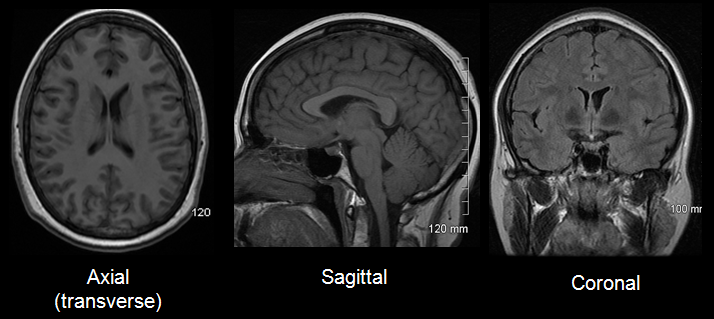
- CT or MRI pictures may be used to check for abnormal areas.

Brain MRI In some cases, blood tests, genetic tests, cerebrospinal fluid (CSF, which is brain fluid) tests are necessary.
How is epilepsy treated?
The goal of treatment is to try to stop seizures completely.
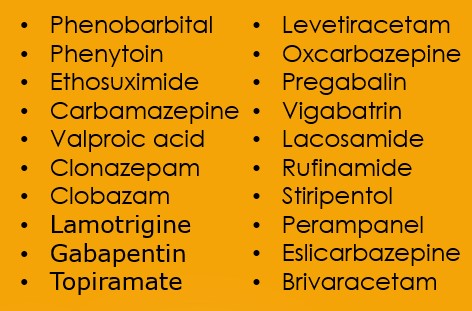
- Medications used to prevent epileptic seizures are called antiepileptics (AEDs). There are over 30 different antiepileptic drugs, but they do not all treat the same types of seizures. Often times obtaining seizure control through antiepileptic drugs is a matter of finding the combination, schedule, and dosing of medications that is right for the individual.
- In some epilepsies, AED is not needed.
- In some epilepsies, person needs to take AED for the rest of his life.
- In majority of cases, if a person is seizure free for several years, a physician may reduce or even stop the person’s medication.

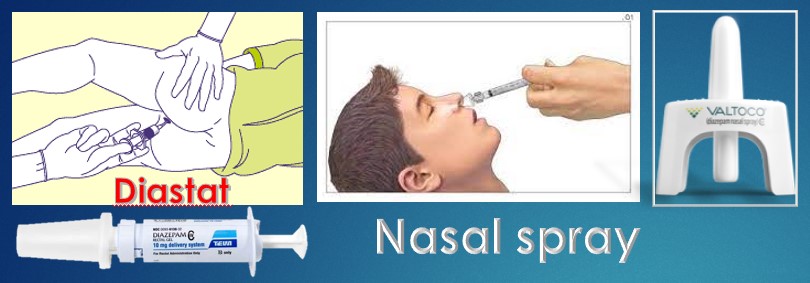
- Emergency seizure medications: if seizure lasts longer than 5 minutes, certain medications are prescribed to stop the seizure. Examples are: Diastat (given rectally), Valtoco, Versed nasal spray.

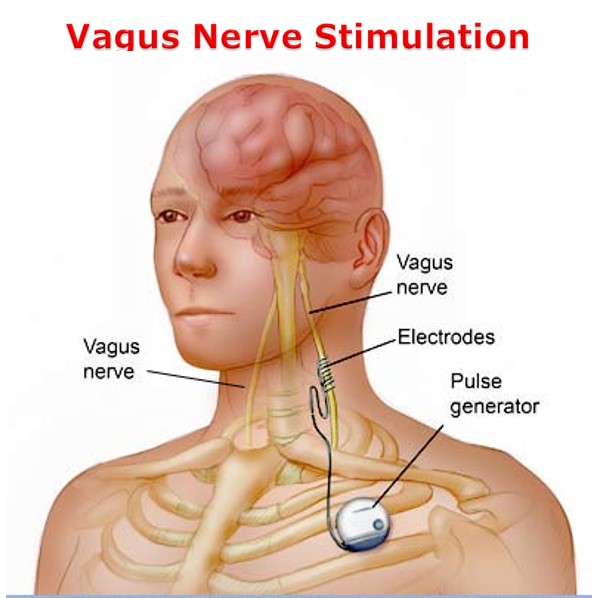
- The Vagus Nerve Stimulator is a device that is implanted in a person. Electrical stimulation of the vagus nerve can reduce the number of a certain type of seizures by more than one half in some people. This treatment is used when seizures continue despite use of AEDs and when surgery is not a possibility.

- A ketogenic diet, which is a very high in fats and low in carbohydrates, may be needed to control the seizures if medicine does not work. The diet may be suggested by the healthcare provider and monitored by a dietitian. It makes the body burn fat for energy instead of glucose.
- In certain conditions, surgery may help reduce how often the person has seizures if medicine does not help.
Complications of epilepsy:
- Status epilepticus: This condition occurs if seizure activity lasts more than five minutes or if you have frequent recurrent seizures without regaining full consciousness in between them. People with status epilepticus have an increased risk of permanent brain damage and death.
- Sudden unexplained death in epilepsy (SUDEP) is a rare complication of epilepsy. In 1 year, 1 child in 4,500 children with epilepsy will have this complication. The risk of SUDEP increases if your child has 3 or more generalized tonic-clonic seizures in 1 year. The risk also increases if person has nocturnal seizures (seizures during sleep). After a nocturnal seizure, breathing can become shallow.
What to do when your child is having a seizure?
- Do not panic.
- Note the start time of the seizure. Record how long it lasts. If possible, videotape the seizure which can be very helpful to his doctor.
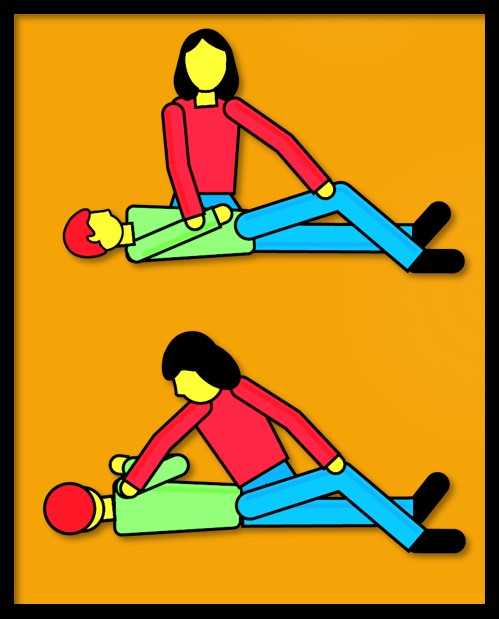
- Gently guide your child to the floor or a soft surface. Cushion child’s head and remove sharp objects from the area around him or her.
- Place your child on his or her side to help prevent him or her from swallowing saliva or vomit.
- Loosen the clothing around your child’s head and neck.

- Remove any objects from your child’s mouth. Do not put anything in your child’s mouth. This may prevent him or her from breathing.
- Let your child sleep or rest after his or her seizure. He or she may be confused for a short time after the seizure. Do not give your child anything to eat or drink until he or she is fully awake.
- If your child has the diagnosis of epilepsy and his doctor has prescribed him a rescue medication to stop the seizure, use it as instructed.
Call local emergency number (911 in USA):
- The person has never had a seizure before.
- The person has difficulty breathing or waking after the seizure.
- The seizure lasts longer than 5 minutes.
- The person has another seizure soon after the first one.
- The person is hurt during the seizure.
- The seizure happens in water.
- The person has a health condition like diabetes, heart disease
Seizure precautions:
- Your child must wear a helmet when he or she rides a bike, scooter, or skateboard.
- Do not let your child sleep on the top of a bunk bed.
- Do not let your child climb trees or rocks.
- Do not let your child lock his or her bedroom or bathroom door.
- Do not let your child swim without an adult who is informed about his or her condition. Have your child use a flotation device, such as a life jacket.
- Tell your child’s teachers and babysitters that he or she has epilepsy. Give them written instructions to follow if he or she has another seizure (a seizure action plan).
- Your child must take showers instead of baths.
Tips to the parents:
- Have your child take his or her medicine every day at the same time. This will also help prevent medicine side effects. Set an alarm to help remind you and your child to take the medicine every day.
- Help your child manage stress. Stress can be a trigger for seizures. Encourage your child to exercise. Exercise can help reduce stress.
- Set a regular sleep schedule. A lack of sleep can trigger a seizure. Try to have your child go to sleep and wake up at the same time every day. Keep your child’s bedroom quiet and dark.
- Keep a seizure diary. This can help you find your child’s triggers and avoid them. Write down the dates of the seizures, where your child was, and what he or she was doing. Include how your child felt before and after. Possible triggers include illness, lack of sleep, hormonal changes, lights, or stress.
- Talk to your child’s family, friends, and school officials about the epilepsy. Give them instructions that tell them how they can keep your child safe during a seizure.
- Your adolescent may not be able to drive until he or she is seizure-free for a period of time. You will need to check the law as it varies from state to state.
- Have your child wear medical alert jewelry or carry a card that says he or she has epilepsy.
 References:
References: